|
3/31/2024 0 Comments What results from scid 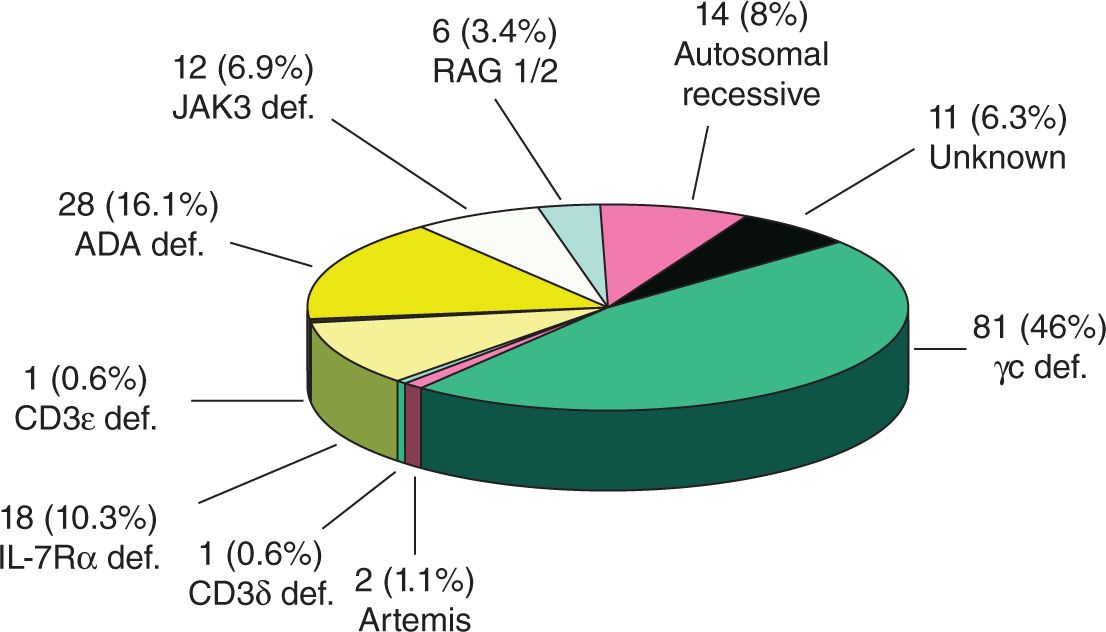
If prenatal testing has not been performed, an at-risk newborn male should immediately be placed in a safe environment and tested for the familial IL2RG pathogenic variant to allow earliest possible diagnosis and treatment. If HSCT involved conditioning chemotherapy, long-term monitoring of vital organ function and neurodevelopmental progress is also warranted.Īgents/circumstances to avoid: To ensure the safety of affected individuals of all ages pending definitive treatment to achieve immunocompetence, parents and other care providers need to assure that the following are avoided: breast-feeding and breast milk (pending clarification of maternal CMV status) exposure to young children, sick persons, or individuals with cold sores crowded enclosed spaces live viral vaccines for the affected individual as well as household contacts transfusion of non-irradiated blood products areas of construction or soil manipulation.Įvaluation of relatives at risk: When the IL2RG pathogenic variant causing X-SCID in the family is known, prenatal testing of at-risk male fetuses may be performed to help prepare for optimal management of an affected infant at birth. Surveillance: After successful HSCT, routine monitoring of affected males every six to 12 months regarding lineage-specific donor cell engraftment growth, immune, and lung function and any gastrointestinal and/or dermatologic issues. Treatment depends on the degree of infectious complications and the presence of immune dysregulation and/or autoimmunity, and requires subspecialty immunologic care to assist in the diagnosis and choice of antimicrobial and immune-suppressive therapies. No: non SCID T Cell Lymphopenia** or secondary causes of TCL*** or idiopathic TCL.Atypical X-SCID. Ideally undertake a definitive procedure within 3 months of diagnosis of SCID Seek advice from SCID centre about starting co-trimoxazole, fluconazole, and immunoglobulin prophylaxis Obtain consent for genetic testing to identify the specific SCID typeĭetermine maternal CMV IgG status on a fresh blood sample to be able to advise about breast feeding – discontinue breast feeding until results available Refer patient immediately to SCID transplant centre Send letter to parents (copying in their GP) using the SCID not found letter template for immunology services which includes advice about immunisations. Yes: see and reassure parents, discharge child. *Flow cytometry normal is defined as >=1,500 CD3/µl AND naïve T cell >=70% Make sure CIS informs researchers of family contact details The same day or within 1 working day of taking diagnostic samples, you should:Ĭommunicate results to family with an informed expert Note: 0.5 ml EDTA blood will be collected and analysed by flow cytometry using the following markers: CD3, CD19, CD56/16, CD4, CD8, CD45RA, CD27 and DR to detect T cells, B cells, NK cells, CD4 T cells, CD8 T cells, naïve T cells and MHC II expression 4. Take a blood sample for the SCID screening lymphocyte subset (see note below) and send to the SCID diagnostic or immunology laboratoryĬonfirm their agreement to be contacted to discuss their experience and follow-up outcomes Of the SCID investigation and explain about flow cytometryĪbout the storage, use and analysis of their baby’s data The appointment should be face to face, unless the baby is in hospital – in which case it should be conducted virtually. The first appointment should be arranged with an informed expert within 2 working days of contacting the family. Liaise with the local hospital for review and management, if baby is unwell or in hospital  
Send confirmation email following phone call using the template for immunology services and teams Phone family and give SCID screening result following the checklist for immunology services Organise an appointment for the baby and their family The following urgent actions should be completed on the same day as the initial notification (not on Friday if the baby cannot be reviewed the next day). Laboratory notifies SCID clinical immunology service ( CIS) as per local protocol on the day of the screening result. Immunology services and teams can use this information to make sure that the babies who need diagnostic testing for SCID are referred and tested in the correct timescales and consistently. A description of the process for babies who are screen positive for severe combined immunodeficiency ( SCID) following routine NHS newborn blood spot ( NBS) screening and are referred into diagnostic services. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
